Is ophthalmology approaching the end of LASIK?
Lenticule extraction poses a provocative question–and a complicated answer
Over the course of 40 years, LASIK has become a household term as millions undergo the procedure each year. Young ophthalmologists have not existed in a world without the refractive surgery, which has improved exponentially since its inception. The LASIK of today is more precise and more effective than ever thanks to advancements like femtosecond lasers and
topography-assisted procedures.
But recent developments in the ophthalmic space, in time, could render LASIK obsolete. That’s the thesis explored by Jod Mehta, PhD, FRCOphth, who is the Distinguished Professor in Clinical Innovation in Ophthalmology at Singapore National Eye Centre, in a presentation at the 2023 British Society of Refractive Surgery (BSRS) meeting, held in July at Said Business School, University of Oxford, England.
At the BSRS meeting, Professor Mehta delivered the Charles McGhee Lecture, titled “Lenticule Extraction: Will LASIK Cease to Exist?” Following the meeting, Professor Mehta spoke with Ophthalmology Times Europe to discuss his presentation and share figures that demonstrate the strengths and limitations of lenticule extraction.
Figure 1. SMILE growth in numbers over years.

“It’s quite a good time to examine whether we should actually be doing LASIK at all,” Professor Mehta said. He cited the growing prevalence of lenticule extraction as a myopia treatment option as a potential threat to LASIK’s dominance in the market. In his BSRS presentation, Professor Mehta catalogued the past decade’s advances in small incision lenticule extraction (SMILE) (Figure 1).1 “It’s an interesting time to examine the way what we call ‘second-generation lenticule extraction’ is going as well,” he added.
Since the late 1990s, he said, patient outcomes from LASIK have vastly improved, thanks to advances in laser technology and innovative applications of refractive surgery techniques. This has resulted in plenty of innovation in the refractive surgery space, but few challengers to LASIK’s market dominance. “When you introduce a new procedure, you’re competing against procedures that already have very, very high standards of outcome,” he explained. “Your margins of improvement have got to be small, single-digit percentages of improvement.” A slim margin of unsatisfied patients, Professor Mehta said, has driven the exploration of alternatives to LASIK. He listed flap trauma, postoperative ocular surface disease, regression and neuralgia as examples of undesirable adverse effects that have incentivised researchers to expand the adoption of lenticule extraction.
Figure 2. SMILE outcomes.
CT, comparative trial; RCT, randomised comparative trial; NOS, Newcastle-Ottawa Scale
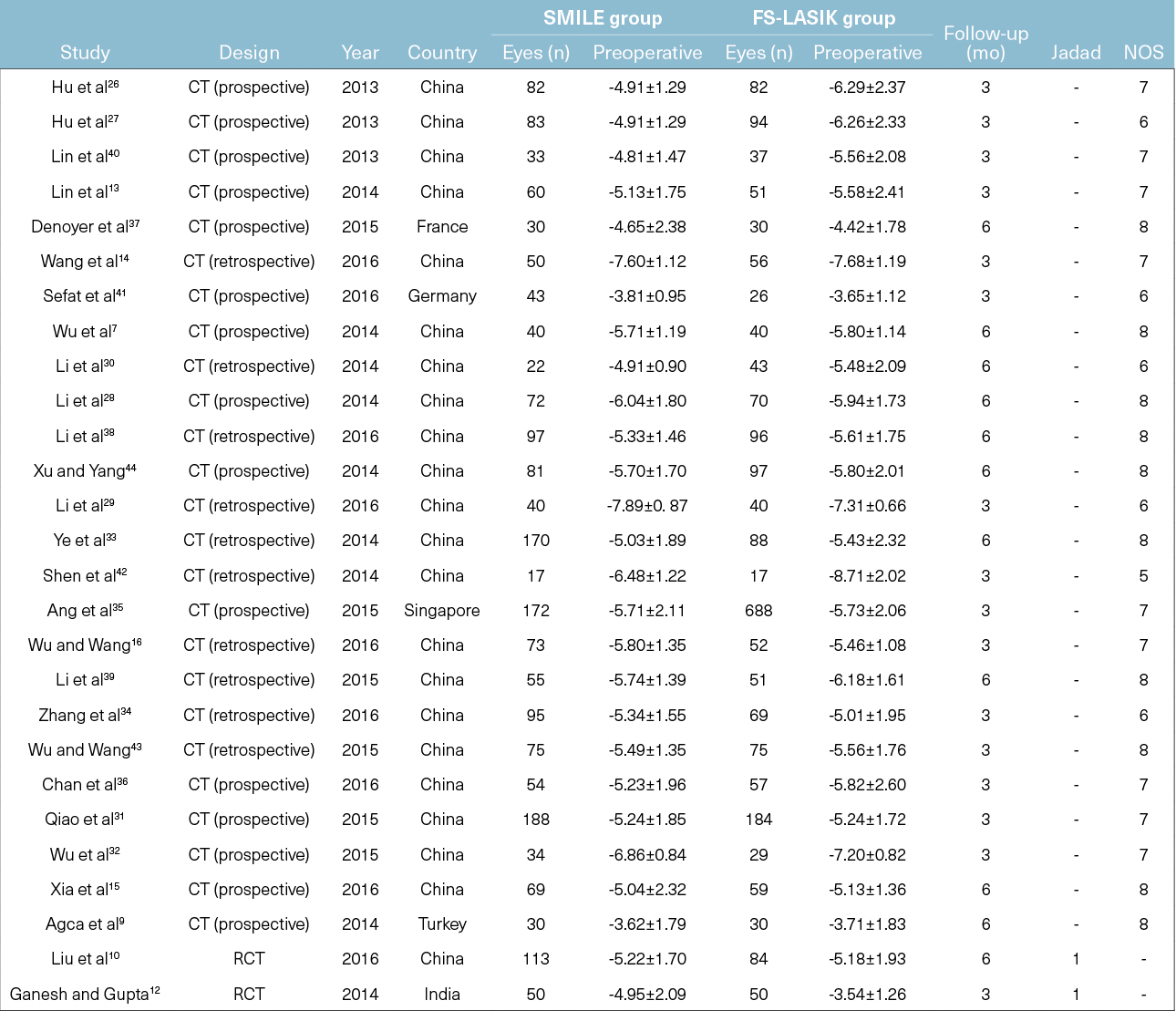
Over time, attempts to eliminate the dissatisfactory effects of LASIK have broadened lenticule extraction from a niche procedure into one with broader refractive applications. Professor Mehta went on to cite recent studies, including his own randomised trial, that have demonstrated no significant difference in final outcomes between lenticule extraction and LASIK.2,3 In the study Professor Mehta coauthored, patients underwent LASIK in one eye and lenticule extraction in the other. “Overall, the data showed with lenticule extraction you could get equivalent results to LASIK, but there was quite a bit of variability,” he said (Figure 2). Professor Mehta cited a lack of centration control and torsion control as major contributors to the variations in “first-generation” SMILE procedures. However, he said, long-term stability seems to have significant improvement in SMILE compared with LASIK, which could eliminate one of the major dissatisfactory outcomes for refractive patients.
Recovery time is another area where lenticule extraction may hold an advantage over even the most modernised LASIK procedures. Many of the devices on the front line of “second-generation” lenticule extraction make use of lower energy. That means less risk of aberrations, Professor Mehta said, and fewer postoperative complications. “There are some data showing having low energy will speed your recovery following lenticule extraction itself,” he said. The primary question, then, becomes one of technique. Professor Mehta said that in most instances, it can be difficult to balance the speed of lenticule extraction with the risk of suction loss. “It’s a balance as to whether you go for lower suction and faster speed, or will you go for lower speed but higher suction,” he said. Approaching lenticule extraction with lower suction but faster speed poses a different problem. The speed of the procedure—often just 10 seconds to cut the whole of the lenticule—leaves no room for correction if there’s an error.1 “You can’t abort the procedure,” Professor Mehta said.
Figure 3. Guiding tunnels: reducing learning curve.
(Figures courtesy of Jod S. Mehta, PhD, FRCOphth)
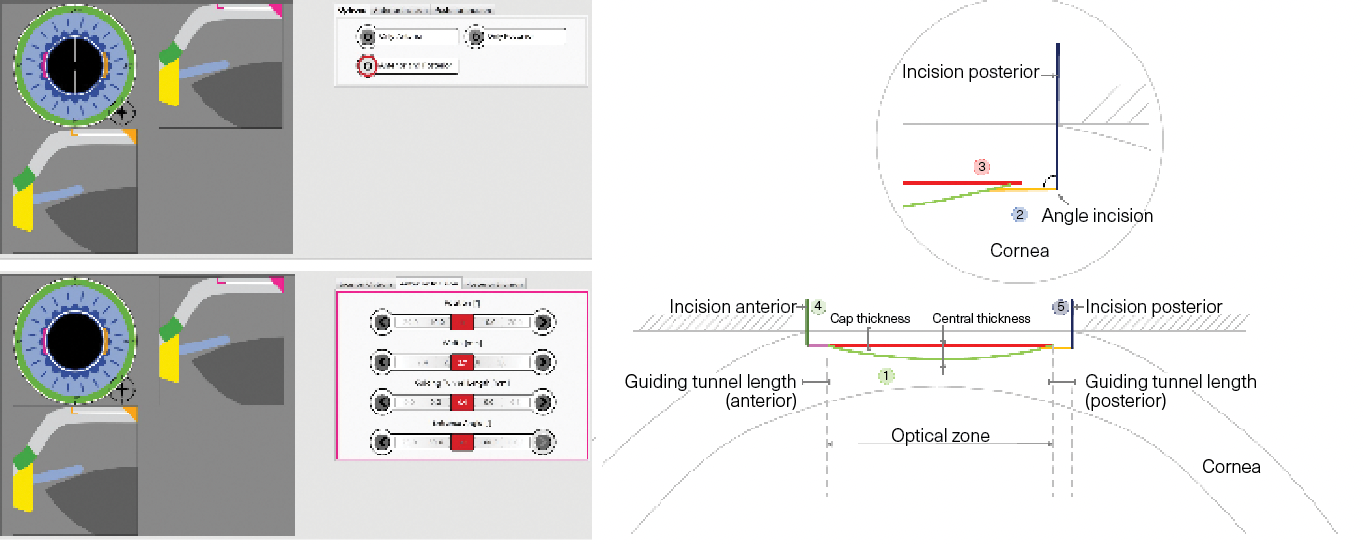
Reviewing current femtosecond laser systems, including the Visumax 800, Schwind FS Laser and Z8 FS Laser, Professor Mehta pointed out the advancements already addressing problems raised in “first-generation” machines.1 New machines are expected to integrate topography units in a way that “basically eliminates” existing performance variations. “With this, you should get superior centration control and torsion controls,” he said. Those controls, along with other innovations in the procedure, could drastically reduce the physician learning curve, Professor Mehta said. For example, the Z8 CLEAR procedureenables physicians to make both an anterior and posterior incision. These “guiding tunnels” provide more control over the lenticule edge (Figure 3). He also predicted more widespread adoption of lenticule extraction as the market diversifies. Physicians are far more likely to make regular use of the procedure when they encounter a device that works for their practice’s needs.“There are other factors as to why people will choose one lenticule machine over another,” Professor Mehta said. “It’s not necessarily related just to outcomes.”
These advances hint at a promising future for lenticule extraction, but do not necessarily indicate an inevitable obsolescence of LASIK. Professor Mehta illuminated the limitations of lenticule extraction procedures, chief among them the restrictions on hyperopic corrections. “Don’t throw LASIK away because you’re not going to be able to do this through current lenticule extraction,” he warned. Currently, there is no approved hyperopic software programme for lenticule devices, so many physicians have been finding workarounds. “What a lot of people do for hyperopic eyes is lenticule addition, where they implant the lenticule to correct the hyperopia,” Professor Mehta said. But that approach is not a universal success, and is representative of the limitations from the relatively new technology. He also pointed at the topography-guided systems currently in place in most lenticule extraction machines, which are not comparable to topography-guided LASIK. “You can’t get that with the current systems,” he said. “Until we have a lenticule machine that can do this in a reproducible manner, we will still have LASIK.”
Still, Professor Mehta said, the ophthalmic world is likely to see a major shift away from LASIK in the next decade, in lieu of a complete desertion. “Myopic LASIK may go down dramatically in the next few years,” he said. And just like LASIK before it, lenticule extraction may explode in popularity as more companies invest in developing the technology. “In 4 or 5 years’ time, if all these companies shift and develop hyperopic software, you may have a bit more challenge to LASIK,” he said.
References
1. Jod M. Will LASIK cease to exist? Charles McGhee lecture presented at: BSRS 30th Annual Scientific Congress; July 9, 2023; Oxford, United Kingdom.
2. Dishler JG, Slade S, Seifert S, Schallhorn SC. Small-incision lenticule extraction (SMILE) for the correction of myopia with astigmatism: outcomes of the United States Food and Drug Administration premarket approval clinical trial. Ophthalmology. 2020;127(8):1020-1034. doi: 10.1016/j.ophtha.2020.01.010.
3. Ang M, Farook M, Htoon HM, Mehta JS. Randomised clinical trial comparing femtosecond LASIK and small-incision lenticule extraction. Ophthalmology. 2020;127(6):724-730. doi: 10.1016/j.ophtha.2019.09.006.
Prof Jod S. Mehta, PhD, FRCOphth
E: jodmehta@gmail.com
Prof Jod S. Mehta BSc (Hons.), MBBS, PhD, FRCOphth, FRCS(Ed), FAMS, FARVO, is the Distinguished Professor of Clinical Innovation and Executive Director of Singapore Eye Research Institute. He is also a senior consultant at Singapore National Eye Centre.

Newsletter
Get the essential updates shaping the future of pharma manufacturing and compliance—subscribe today to Pharmaceutical Technology and never miss a breakthrough.